Consent in question as students face the regulator
Harry McCay, BComm, LLB, Special Counsel, Avant Law
Thursday, 30 November 2023
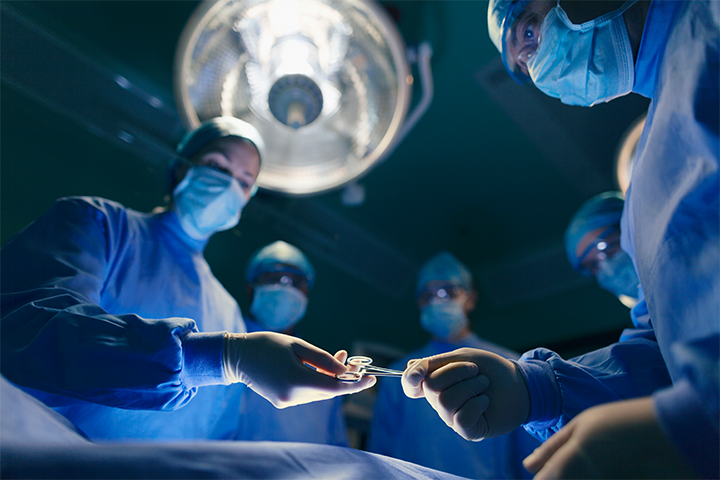
We supported a number of medical students facing disciplinary proceedings after they examined an unconscious patient in the operating theatre. The examination was not part of the procedure but done under the direction from their supervising surgeon to demonstrate their skills for a particular part of their training.
Often, it’s a nurse or anaesthetist who makes the complaint, and in this case a nurse objected at the time of the examination but was overruled by the surgeon.
During disciplinary proceedings, students were asked why it didn’t occur to them that consent may not have been obtained, and why they didn’t ask more questions before complying with the supervisor’s instruction.
Consent is a challenging area of medico-legal law and doctors can struggle with it at any point in their careers. So, what are the consent issues you need to be aware of in the operating theatre?
All along you’ve been taught about the importance of consent
You are carefully instructed in your pre-clinical years about the importance of obtaining consent from patients before taking a history or performing an examination. You are taught to introduce yourself both by name and by role before asking permission to interact with a patient.
How do you apply this in the operating theatre with an unconscious patient?
Students must rely on hospital process and be comfortable that their supervisor has discussed with the patient that students may be present during their procedure. Students have to assume their supervisor has obtained specific permission for any examination by the student or involvement in the procedure in their consent discussions with the patient.
If it’s not a standard part of the procedure, you need consent
As treatment is provided by a team of people in public hospitals, it may well be that ordinary consent to undergo, for example, a laparoscopic procedure is sufficient to cover a student holding equipment or doing some part of the procedure.
The difficulty comes if you are directed to perform an examination which is not necessarily part of the treatment, but solely for you to learn a clinical skill.
While this has been accepted as part of a doctor’s training for over a century, because it’s not part of the operative procedure it’s not covered by standard consent.
If your clinical supervisor instructs you to examine a patient who is unconscious, a number of issues arise:
- you’re unable to get consent from the patient
- you don’t know what was discussed with the patient during the consent process
- a significant power imbalance exists between you and your supervisor
- you probably only have seconds to decide what to do.
Where do you stand?
It’s the university’s responsibility to ensure training supervisors don’t direct students to contravene the Medical Board of Australia’s Good medical practice: a code of conduct for doctors in Australia.
However, as a student you should be able to recognise a request where consent may not have been obtained and question this. Ultimately, it’s up to you to abide by the code.
Three things you can do:
- Familiarise yourself with our factsheet Consent essentials.
- Be willing to respectfully challenge an instruction which is at odds with your training.
- If you have any concerns, contact Avant for assistance and advice.
How Avant supports students in disciplinary proceedings
Avant has helped a number of student members with complaints regarding consent. We ensure they are treated fairly and argue that a their junior position in the theatre during training can make their ability to question or refuse, extremely difficult.
Medical students often ask us, ‘Why do I need insurance?’ This example is a very good reason why it pays – or not, since student membership with Avant is free.
More information
For medico-legal advice, contact us on nca@avant.org.au or call 1800 128 268, 24/7 in emergencies.
IMPORTANT: This article is not comprehensive and does not constitute legal or medical advice. You should seek legal or other professional advice before relying on its content, and practise proper clinical decision making with regard to the individual circumstances. Persons implementing any recommendations contained in this article must exercise their own independent skill or judgement or seek appropriate professional advice relevant to their own particular practice. Compliance with any recommendations will not in any way guarantee discharge of the duty of care owed to patients and others coming into contact with the health professional or practice. Avant is not responsible to you or anyone else for any loss suffered in connection with the use of this information. Information is only current at the date initially published. © Avant Mutual Group Limited 2023