
Diagnostic error in claims
| Overview | Practice points |
|
|
All data is based on Avant claims and complaints closed from 1 July 2019 to 30 July 2024.
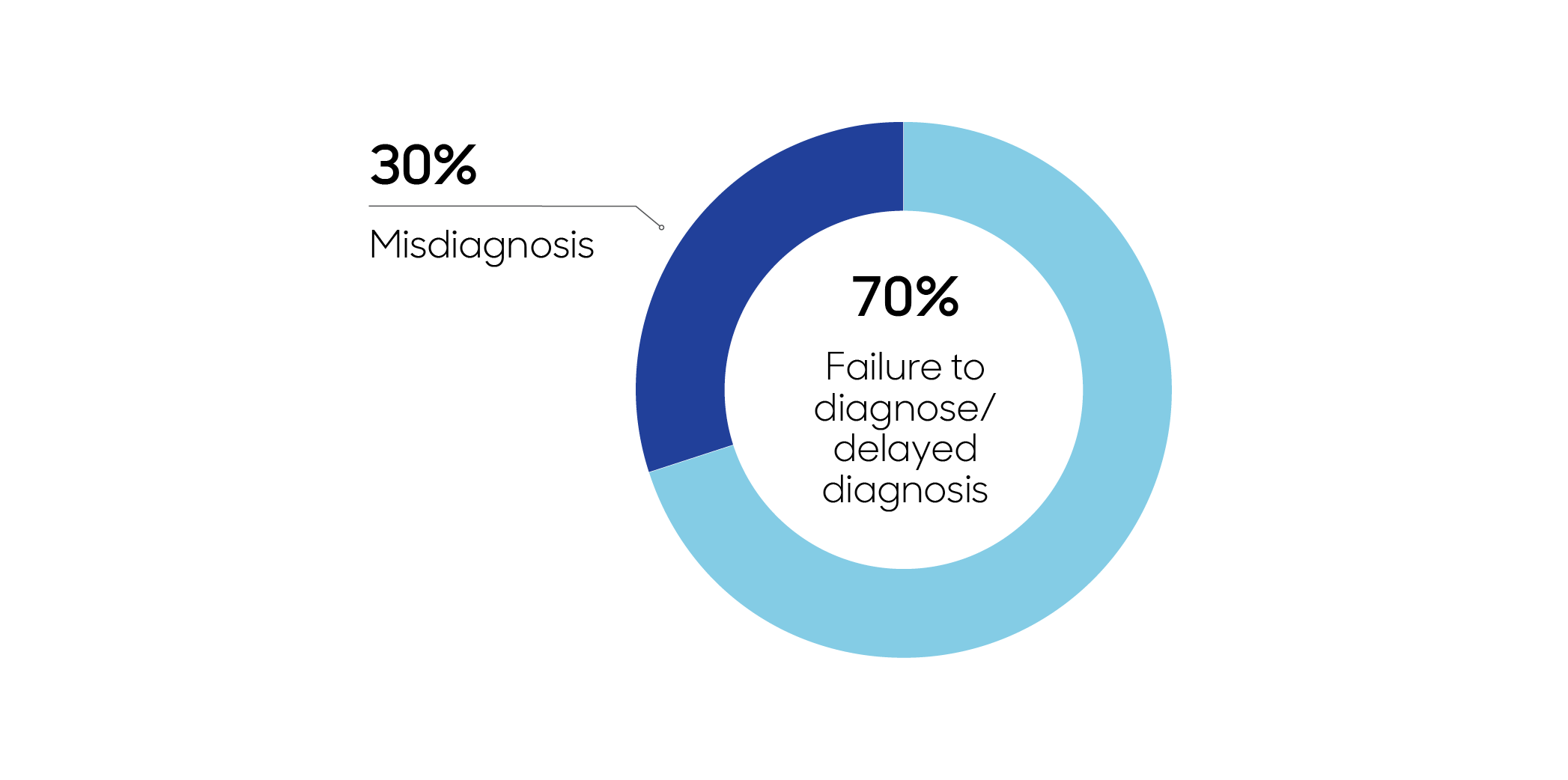
1 in 6 claims were primarily about diagnostic error.
In these claims, failure to diagnose a patient’s condition, or delay in the diagnosis were much more common issues than misdiagnosis.
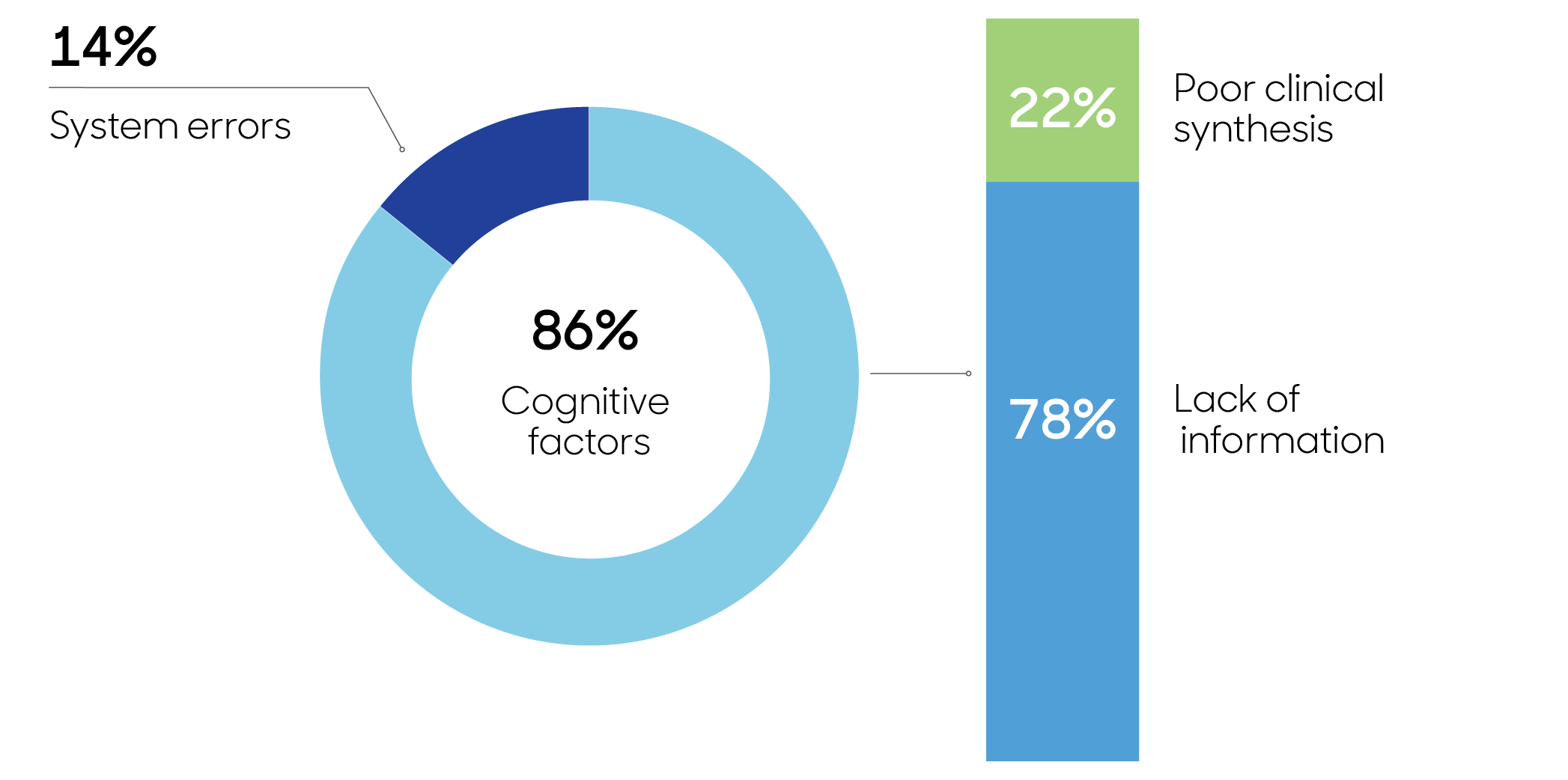
In 86% of diagnostic error claims, cognitive factors were the main error identified.
The predominant issue was lack of information required in decision-making. This was often a result of:
- inadequate examination
- delay or failure to refer for appropriate diagnostic testing
- failure to heed patient complaints or symptoms
- inadequate history.
Poor clinical synthesis was a less common issue, often a result of incorrect image interpretation or failure to establish a differential diagnosis.
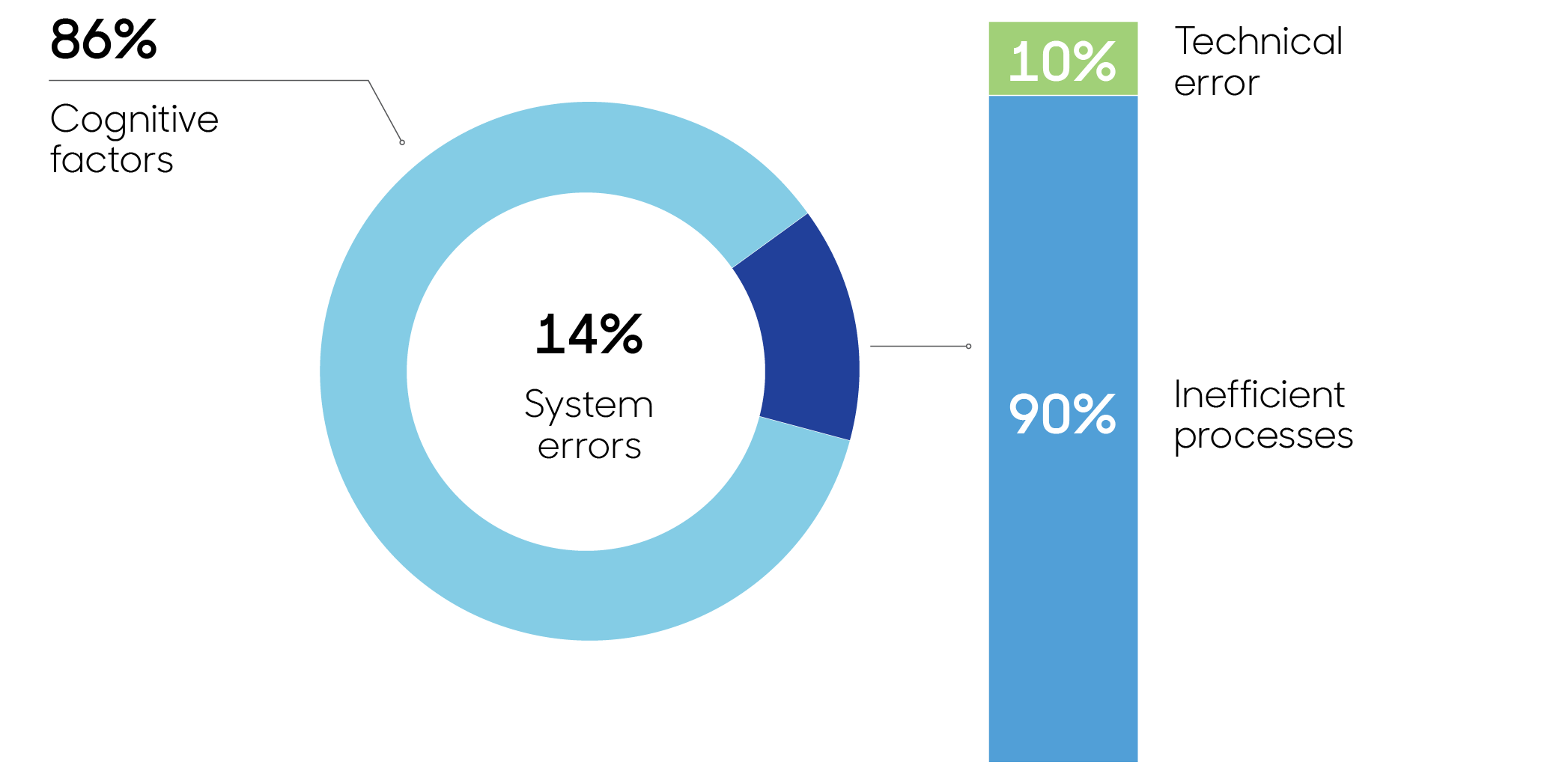
System errors were shown to be the main error in 14% of diagnostic error claims.
Most of these issues indicated inefficient processes that contribute to diagnostic error. Most common were:
- delay or failure to follow-up tests/investigations
- failure to action results of tests, investigations or referral recommendations
- failure to follow-up patient/referral.
Technical errors were less reported. These included incorrect transcription of image reports and other errors in the handling and processing of diagnostic tests and reports.
Communication
Poor communication was an additional allegation in one-third of diagnostic error cases. These involved issues with both the content and manner of communication:
- The failure to communicate results and information to patients, families, or external healthcare providers was a predominant issue.
- The manner of communication was of significant concern such as in cases where the patient was ignored, dismissed, intimidated, or felt a lack of empathy from the doctor.
(The above incidence was based on cases that had diagnostic error issues as the primary allegation and communication issues as a secondary allegation.)
Assessment of the care provided
Experts and/or regulators assessed the care provided in diagnostic error claims, with the following results:

About this analysis
This report is based on our analysis of the underlying themes of claims for Avant member doctors from all specialties and practices, including complaints to regulators and compensation claims finalised between 1 July 2019 and 30 June 2024.
Analysis of claims with diagnostic error was based on more than 2,000 claims and complaints with a diagnostic error issue as the primary allegation.
More information
For medico-legal advice, please contact us here, or call 1800 128 268, 24/7 in emergencies.
For any queries on this analysis, please contact us at research@avant.org.au.
Additional resources
For articles, factsheets, case studies and other resources on a range of topics, including diagnosis, visit the insights & resources page.
IMPORTANT: Avant routinely codes information collected in the course of assisting member doctors in medico-legal matters into a standardised, deidentified dataset. This retrospective analysis was conducted using this dataset. The findings represent the experience of these doctors in the period of time specified, which may not reflect the experience of all doctors in Australia. This publication is not comprehensive and does not constitute legal or medical advice. You should seek legal or other professional advice before relying on any content, and practise proper clinical decision-making with regard to the individual circumstances. Persons implementing any recommendations contained in this publication must exercise their own independent skill or judgement or seek appropriate professional advice relevant to their own particular practice. Compliance with any recommendations will not in any way guarantee discharge of the duty of care owed to patients and others coming into contact with the health professional or practice. Avant is not responsible to you or anyone else for any loss suffered in connection with the use of this information. Information is only current at the date initially published [August 2025].
